Connecting a Nation: Bringing care to remote villages in Bhutan through WTI's Hub and Spoke Model
Central Regional Referral Hospital in Gelephu, Bhutan
In many parts of the world, access to healthcare depends heavily on geography. If you’re lucky to live near a larger city, you may be able to see a medical specialist, but this leaves rural communities without access. Many families don’t have transportation and cannot get to the healthcare they need that is hours or even days away.
How the hub and spoke model expands access
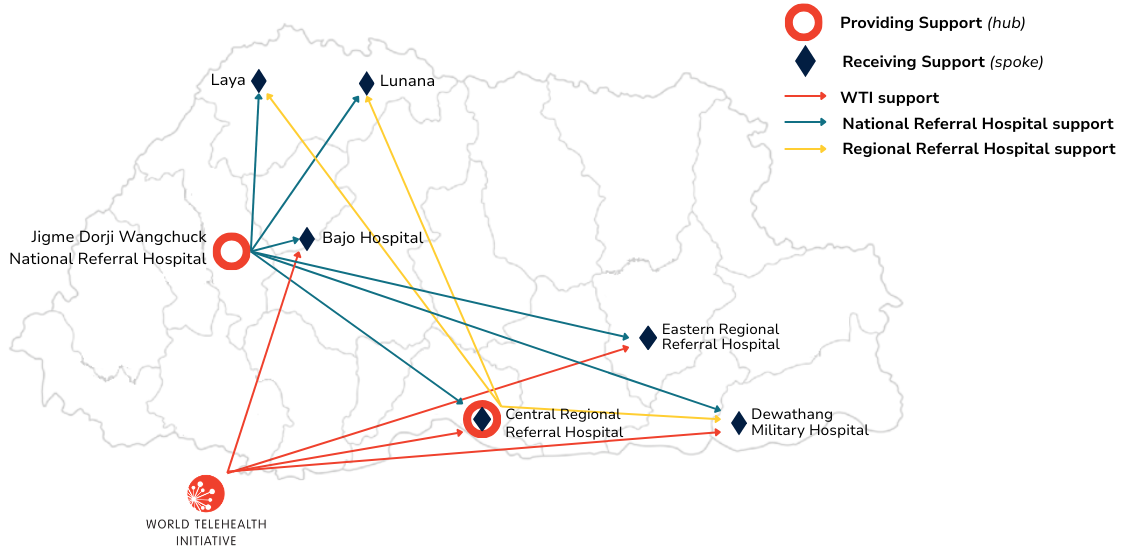
WTI’s hub and spoke model strengthens care across regions by connecting referral hospitals with smaller health centers through telehealth. National and regional hospitals serve as hubs, providing specialist support to surrounding facilities with fewer resources. When a complex case arises, clinicians at a spoke site can consult with specialists at the hub in real time. Hubs and spokes can also connect with WTI’s global corps of volunteer specialists when additional expertise is needed. This reduces unnecessary referrals, eases pressure on national hospitals, and keeps more care within local communities.
Bhutan: Building a national telehealth network
In the Kingdom of Bhutan, a small country in the Himalayas, WTI is working with local healthcare leaders to build a coordinated telehealth network that reaches across the country, including extremely remote communities that have little to no healthcare access.
WTI’s program connects medical specialists at Jigme Dorji Hospital, the country’s largest hospital with the most specialists, to other hospitals across the country. Through telehealth, psychiatrists, critical care physicians, and other specialists provide bedside support, case review, and training to clinicians outside the capital. Expertise that was once concentrated in the capital city now reaches facilities across the country.
The program is designed by Bhutanese leadership to best meet the country’s health needs and maximize their existing resources. Two of the greatest areas of need are ICU care and Psychiatry. There are only five psychiatrists and five intensivists in Bhutan, all located at Jigme Dorji Hospital in the capital.
Reaching remote communities with psychiatric care
The spoke sites include extremely rural communities such as Lunana and Laya. Lunana is so remote that it can only be reached on foot. A community health worker comes to visit the village once a month and sees patients, otherwise the community has no access to healthcare. There is a community health worker and general practitioner stationed in Laya, but health services are limited and any sort of specialized care is out of reach.
WTI donated telehealth devices to Laya and Lunana, which will be used for regular psychiatry clinics. A psychiatrist at Jigme Dorji will connect into the device to see patients who need psychiatric care, and WTI’s entire corps of medical specialists can also support the community health worker with care needs.
Strengthening ICU care across the country
Bhutan recently instituted a national directive requiring specialist oversight for all ICU patients. Several hospitals have ICUs but no intensivists. Asynchronous ICU support from the capital is slow and not ideal for patients in critical condition. By linking hospitals to the intensivists at Jigme Dorji Hospital through a coordinated telehealth network, the hub-and-spoke structure allows specialists to examine the patient via telehealth and discuss the care plan with local providers. This will greatly improve the support for patients.
Long term system impact
Training is central to the model’s long-term success. As clinicians participate in consultations and ongoing case discussions, they build practical skills and confidence. Over time, experienced providers begin supporting additional sites, creating a train-the-trainer effect that expands capacity within the national workforce. The network becomes stronger as local expertise grows.
WTI’s program in Bhutan illustrates how thoughtful expansion can strengthen a country’s healthcare system. By aligning telehealth with national health policy and embedding it into routine care pathways, the hub-and-spoke model expands specialty access, supports local clinicians, and builds capacity across the country.
As WTI continues to grow, this model remains central to our work: connecting hubs to spokes, strengthening health systems, and expanding access to specialty care across countries and regions.